|
E-Mail Edition Volume 7 Number 1 |
|||
|
Originally published Winter, 2010 Published by Piccadilly Books, Ltd., www.piccadillybooks.com. Bruce Fife, N.D., Publisher, www.coconutresearchcenter.org |
|||
|
If you would like to subscribe to the Healthy Ways Newsletter
|
Contents
|
||
|
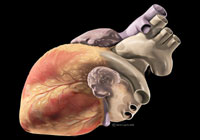
Human Heart Patrick J. Lynch, medical illustrator
|
New Study Shows Coconut Oil Protects Against Heart Disease, Diabetes, and Obesity
A new study published in the scientific journal Lipids demonstrates that coconut oil consumption raises HDL (good) cholesterol, lowers the cholesterol ratio (reducing risk of heart disease), improves blood sugar levels, decreases risk of diabetes, decreases body fat, reduces abdominal circumference, and can aid in fighting overweight and obesity. A number of previous studies, mostly using fractionated coconut oil (i.e. medium chain triglyceride oil) have demonstrated similar results. This study, however, measured the effects of various health parameters using ordinary coconut oil. One of the criticisms skeptics have used to refute the claims for the health benefits of coconut oil is that the majority of the studies didn't directly test coconut oil but tested fractionated coconut oil, which is also known as MCT oil. Natural coconut oil contains a total of 10 fatty acids, 63 percent of which are medium or short chain fatty acids. MCT oil, on the other hand, consists primarily of only two medium chain fatty acids (MCFAs). When MCT oil is produced, coconut oil is fractionated or divided into the different fatty acids. All but two, caprylic and capric acids, are removed. Ironically, when MCT oil is produced, the most important MCFA, lauric acid, is removed. Even without lauric acid, MCT oil has shown to have many health benefits. Anti-saturated fat proponents have claimed that the benefits produced by MCT oil cannot be equated with coconut oil. They acknowledge that the two MCFAs in MCT oil may have health benefits, but that coconut oil, consisting of 10 fatty acids, would not have the same benefits. This study disproves their claim. The study examined the effects of coconut oil supplementation on women with abdominal obesity—that is, a waist circumference greater than 35 inches (88 cm). The study compared 40 women between the ages of 20 and 40 years of age. Twenty women were supplemented with 30 mL (2 tablespoons) of coconut oil and 20 women received 30 mL of soybean oil daily over the course of 12 weeks. The subjects were also instructed to follow a balanced, low-calorie diet and to walk for 50 minutes a day for exercise. Blood cholesterol levels and other measurements were recorded at the beginning and at the end of the study period. Instructed to cut down on calories, participants in both groups reduced overall calorie intake by reducing the amount of carbohydrate they ate. Protein and fiber intake increased slightly while fat consumption remained the same even with the added 2 tablespoons of oil. Each participant consumed the number of calories considered to be ideal for their height, or on average just under 1,900 calories daily. So, participants were not dieting, they were simply eating a little less than they ordinarily did. After 12 weeks, bodyweight and body mass index (BMI) in both groups had decreased. However, only in the group receiving the coconut oil was waist circumference significantly decreased. (In the soybean oil group, waist measurement actually increased.) These changes are very important for several reasons. For one, it indicates that the coconut oil group experienced more fat loss as opposed to protein or water loss. But more importantly, it indicates a reduced risk of diabetes and heart disease in the coconut oil group, but not in the soybean oil group. The group taking the coconut oil had increased levels of the beneficial HDL cholesterol, which is believed to protect against heart disease, and had a lower cholesterol ratio (LDL/HDL). The cholesterol ratio is considered the most accurate indicator of heart disease risk of all the cholesterol measurements. Please take note: this study demonstrates that according to the cholesterol values, coconut oil reduces the risk of heart disease. Here is the proof many critics keep asking for—that is, a double blind study published in peer reviewed, top of the class scientific journal. The subjects taking soybean oil, on the other hand, didn't fare as well. In this group total cholesterol went up, LDL (the bad) cholesterol went up, the cholesterol ratio went up, and the heart protective HDL cholesterol went down—all bad! Each of these changes indicates increased risk of heart disease. Therefore, according to this study soybean oil, a so-called "heart-friendly" polyunsaturated vegetable oil, increases the risk of heart disease while coconut oil protects against it. This study also provides evidence demonstrating that coconut oil protects against metabolic syndrome. Metabolic syndrome (also referred to as syndrome X) refers to an association between certain metabolic disorders and cardiovascular disease and type 2 diabetes. People with metabolic syndrome are at high risk for developing heart disease and type 2 diabetes. This study shows that coconut oil reduces risk of metabolic syndrome and, therefore, protects against both heart disease and diabetes. The American Heart Association and the National Heart, Lung and Blood Institute identify a person as having metabolic syndrome if they have any three or more of the following five conditions:
|
||
|
|
||
The above study demonstrates that those who added coconut oil into their diets showed a decrease in waste circumference, increased HDL, and reduced fasting blood glucose. Triglycerides showed no improvement in either the coconut or soybean oil groups. Blood pressure was not recorded. So, out of the four parameters tested, coconut oil produced improvements in three. Another recent study published last year in the journal Diabetes shows that coconut oil reduces insulin resistance, supporting the findings in this study. This diabetes study was discussed in the previous issue of the Healthy Ways Newsletter (6-5). If you missed the article, you can access it here. Another interesting finding from this diet study was that c-reactive protein (CRP), a marker for inflammation, was significantly reduced in the coconut oil group. Elevated levels of CRP are correlated with increased heart disease risk. In fact, in the Harvard Women's Health Study, CRP levels were more accurate than cholesterol in predicting heart problems. After three years, CRP proved to be the strongest predictor of risk. Women in the group with the highest CRP levels were more than four times as likely to have died from heart attack or suffered a nonfatal heart attack or stroke. This group was also more likely to have required a heart procedure such as angioplasty or bypass surgery than women in the group with the lowest levels. Besides heart disease, inflammation is implicated as a major confounding factor in numerous degenerative diseases including diabetes, Crohn's disease, ulcerative colitis, arthritis, Alzheimer's disease, Parkinson's disease, liver disease, kidney disease—the list goes on and on. Researchers are linking inflammation to an ever-increasing array of chronic illnesses. One class of medications used in treating all of these disorders is anti-inflammatory drugs. Coconut oil offers another means to help control inflammation and fight these diseases. This study verifies previous studies that indicated that coconut oil has anti-inflammatory properties. This is an important issue because coconut oil critics claim, with little justification, that saturated fats promote inflammation. This study demonstrates just the opposite. Once more, it also demonstrates that coconut oil consumption improves cholesterol values and does not promote heart disease. It provides evidence that coconut oil is heart healthy and should be used to fight off heart disease. ■
Reference Assuncao, M.L., et al. Effects of dietary coconut oil on the biochemical and anthropometric profiles of women presenting abdominal obesity. Lipids 2009;44:593-601.
|
|||
|
|
|||
|
Saturated Fats Not Linked to Heart Disease Study Says
Reducing dietary saturated fat has generally been thought to improve cardiovascular health and protect against heart attacks and strokes. This assumption is based on the belief that dietary saturated fat promotes cardiovascular disease. A new meta-analysis study published in the American Journal of Clinical Nutrition says this isn't so. Despite the commonly held belief, saturated fat does not promote heart disease. The idea that fat, particularly saturated fat, consumption was linked to heart disease was instigated by Dr. Ancel Keys. The theory was bolstered in Keys' Seven Countries Study published in 1970. Using data from seven countries (United States, Japan, Italy, Greece, the Netherlands, Finland, and Yugoslavia), Keys showed that the countries that had the highest saturated fat consumption also had the highest number of deaths from heart attacks. This study was used as the standard upon which the medical profession and government health agencies justified their campaign against saturated fat. Keys' study, however, had several flaws, one of which was assuming high saturated fat consumption was directly related to heart disease deaths. Researchers pointed out that there were other factors within these countries that also paralleled the high heart disease rate. One researcher, Dr. John Yudkin, showed that sugar consumption was also high in these countries and fit the pattern just as well as saturated fat. Dr. Yudkin suggested that it was more likely high sugar consumption that was the cause of heart disease and not saturated fat. Indeed, when food consumption data from a number of other countries were analyzed, sugar consumption proved to be a far better indicator of heart disease risk than saturated fat. Over the years, many studies have sought to prove Keys' hypothesis. Results were mixed. Some seemed to support it, while others did not. However, the majority of the medical community, along with the pharmaceutical industry (which profited greatly from the saturated fat-heart disease idea), supported the theory. Those studies that supported Keys' theory received national press and were used as justification to establish government policies on health, while those that did not support the theory were ignored. The evidence in favor of Keys' theory was no greater than the evidence that contradicted it. In fact, there was a substantial amount of evidence that challenged the theory. Some of the studies used relatively few participants, while others used much larger numbers. Obviously, the results of a study involving 50,000 test subjects carried more weight than one involving only 1,000. One large study using 50,000 participants would produce more reliable results than 10 small studies with a total combined number of 10,000 participants. So the total number of studies is not the issue; the number of people in the studies is of more value. If all the subjects in these different studies were combined and evaluated, what would the final outcome be? Would it prove Keys' theory or disprove it? Researchers at the Children's Hospital Oakland Research Institute in California and Harvard School of Public Health got together to find out. They analyzed all the previous studies with data for dietary saturated fat intakes and risk of cardiovascular disease. Twenty-one studies were identified that fit their criteria. This meta-analysis study included data on nearly 350,000 subjects. The focus of the researchers was to determine if there was sufficient evidence linking saturated fat consumption to cardiovascular disease. Their results said "no." Intake of saturated fat was not associated with an increased risk of cardiovascular disease. Those people who ate the greatest amount of saturated fat where no more likely to suffer a heart attack or stroke than those who ate the least. No matter how much saturated fat one ate, the incidence of heart disease was not affected. This study demonstrates that the combined data from all available studies disprove Keys' hypothesis. ■
Reference Siri-Tarino, P.W., et al. Meta-analysis of prospective cohort studies evaluating the association of saturated fat with cardiovascular disease. American Journal of Clinical Nutrition 2010;91:535-546.
|
|||
|
Mycoplasma Infections Photo courtesy of CDC/Dr. Vester Lewis
|
Study Ties Microbes to Premature Births
(Los Angeles Times) Microbes in the wrong place at the wrong time—a woman's amniotic fluid during pregnancy—might play a role in causing premature births, according to a study published in the online journal PLoS ONE. Using a sensitive molecular technique, researchers found a greater quantity and variety of bacteria and fungi in a significant portion of women who gave birth prematurely. The more severe the infection, the earlier the women were likely to give birth. The amniotic sac, which surrounds a fetus in the womb, has long been considered a protected site. "Certain kinds of organisms have been known to get in and not necessarily cause any harm," said Dr. David Relman, an infectious disease specialist at Stanford University School of Medicine and the study's senior author. "But in general, bugs don't belong there." One in eight American infants is born before full term, which is defined as 38 weeks. The high rate is attributed in part to assisted reproduction, which often results in twins or triplets. But the cause of about half of all spontaneous premature births is a mystery. Babies born too early can have learning disabilities, neurological problems, lung diseases and cerebral palsy. Prematurity is the leading cause of infant mortality in the United States, accounting for more than one-third of all infant deaths, according to the national Centers for Disease Control and Prevention (CDC). Dr. Dan GiGiulio, a research associate in Relman's laboratory, used two techniques of molecular biology—polymerase chain reaction and DNA sequencing—to look for microbes in amniotic fluid samples from 166 women in pre-term labor. Of these, 113 went on to deliver prematurely and 53 carried their babies full term. DiGiulio found evidence of infection in 15 percent of the samples, all from women who gave birth early. The microbes found represented one fungal (Candida albicans) and 17 bacterial species, including one that had never been identified, according to the report. One of the most common was Leptotrichia, which can be found in the mouth and the vagina. Both gum disease and bacterial vaginosis have been shown to increase the risks of premature delivery.
Dr. Fife's Comments: Amniotic fluid should be sterile. The way microbes invade the amniotic fluid is through the placenta; indicating that the mother's blood was contaminated with bacteria and fungi. How did these microbes get into the blood? Where did they come from? It is interesting to note that many of the species found in the amniotic fluid are common inhabitants of the mouth. In fact, numerous studies have found that oral bacteria do indeed find their way into amniotic fluid (see references at end of this article). Oral bacteria as well as viruses and fungi in the mouth can seep into the bloodstream quite easily. When periodontal disease or an active infection is present, large amounts of bacteria enter the bloodstream. Even relatively "healthy" mouths can be breeding grounds for bacteria that find their way into the bloodstream. The human mouth harbors billions of bacteria. There are over 600 different species of bacteria which call your mouth their home. With so many bacteria concentrated in one spot, it is easy to see how they can have a detrimental effect on oral health. Despite daily brushing and flossing, over 90 percent of the population has some level of dental decay or gum disease. Consider this fact: one third of people 65 years of age and older have lost all of their teeth due to poor dental health. Our teeth were not designed to fail at a certain age. They were meant to last a lifetime. Apparently, brushing and flossing isn't good enough. Diet is important. When Dr. Weston A. Price traveled the world in the 1930s studying the health and diets of various peoples, he found that those who subsisted on primitive or traditional diets had excellent dental health and died at advanced ages with all of their teeth intact. They had good dental health into old age despite the fact that they didn't brush their teeth, use mouthwash or dental floss, or see dentists. However, when they began to add modern foods into their diets, their dental health declined dramatically. Diet affects the type of microbes that live in our mouths. Sugary foods and refined grains promote the overgrowth of harmful bacteria that promote tooth decay and gum disease. Our modern diet is loaded with sugar, sweets, sweetened beverages, and refined grains. Most of us subsist on foods that promote poor dental health. That is why 90 percent of the population has imperfect oral health. Eating a more traditional diet of whole, fresh foods is one step you can take to improve the health of your mouth. Another step is to add oil pulling to your daily oral hygiene routine. Oil pulling is a method of oral detoxification that has proven to reduce dental plaque and gingivitis better than brushing and using antiseptic mouthwash. Oil pulling shouldn't replace brushing, but it should be a regular part of your daily dental care. Oil pulling is basically rinsing the mouth with vegetable oil, much like you would do with a mouthwash, except you do it for about 15-20 minutes. I prefer to use coconut oil for oil pulling because it provides many health benefits missing from other oils. Oil pulling is best done first thing in the morning before eating breakfast. "Pulling" for 15-20 minutes sounds like a long time, but if you do other things at the same time, such as read the newspaper, fix breakfast, or take a shower, the time goes by fast. When you are finished pulling, don't swallow the oil: it is full of bacteria, pus, and mucus. Spit it out. The way oil pulling works is that it draws or "pulls" bacteria out of the mouth, thus reducing the number of microbes that can cause trouble. This allows tissues in the mouth to heal, thus reducing the amount of bacteria that is absorbed into the bloodstream. |
||
|
Medical research over the past several years has identified several health conditions caused by oral bacteria which migrate to other parts of the body. Besides low-birth weight and preterm births, oral bacteria can cause or exacerbate heart failure, atherosclerosis, diabetes, bronchitis, osteoporosis, arthritis, colitis, and numerous other health problems. If you want to learn more about how oral health affects your entire body I recommend my book Oil Pulling Therapy: Detoxifying and Healing the Body Through Oral Cleansing. In this book I give an in-depth overview of the relationship between oral and systemic health and provide a program using oil pulling, diet, and other procedures to clean the mouth and heal the body. Oil pulling is excellent way for expectant mothers to prevent bacterial infection from attacking developing fetuses and increase chances of having a healthy, full-term delivery. ■
|
|||
|
|
References Wimmer G, and Pihlstrom BL. A critical assessment of adverse pregnancy outcome and periodontal disease. J Clin Periodontol. 2008 Sep;35(8 Suppl):380-97.
Kinane D, Bouchard P; Group E of European Workshop on Periodontology. Periodontal diseases and health: Consensus Report of the Sixth European Workshop on Periodontology. J Clin Periodontol. 2008 Sep;35(8 Suppl):333-7.
Al-Habashneh R, Aljundi SH, Alwaeli HA. Survey of medical doctors' attitudes and knowledge of the association between oral health and pregnancy outcomes. Int J Dent Hyg. 2008 Aug;6(3):214-20.
Williams RC. Understanding and managing periodontal diseases: a notable past, a promising future. J Periodontol. 2008 Aug;79(8 Suppl):1552-9.
Heimonen A, Rintamaki H, Furuholm J, Janket SJ, Kaaja R, Meurman JH. Postpartum oral health parameters in women with preterm birth. Acta Odontol Scand. 2008;66(6):334-41.
Mayer Y, Levin L, Oettinger-Barak O, Machtei E. Pregnancy and periodontal disease—is there a relation? Refuat Hapeh Vehashinayim. 2008 Jan;25(1):24-33, 82.
Horton AL, Boggess KA, Moss KL, Jared HL, Beck J, Offenbacher S. Periodontal disease early in pregnancy is associated with maternal systemic inflammation among African American women. J Periodontol. 2008 Jul;79(7):1127-32.
López R. Periodontal disease and adverse pregnancy outcomes. Evid Based Dent. 2008;9(2):48.
Examining the safety of dental treatment in pregnant women. J Am Dent Assoc. 2008 Jun;139(6):685-95.
Sacco G, Carmagnola D, Abati S, Luglio PF, Ottolenghi L, Villa A, Maida C, Campus G. Periodontal disease and preterm birth relationship: a review of the literature. Minerva Stomatol. 2008 May;57(5):233-46, 246-50.
Silk H, Douglass AB, Douglass JM, Silk L. Oral health during pregnancy. Am Fam Physician. 2008 Apr 15;77(8):1139-44.
Mobeen N, Jehan I, Banday N, Moore J, McClure EM, Pasha O, Wright LL, Goldenberg RL. Periodontal disease and adverse birth outcomes: a study from Pakistan. Am J Obstet Gynecol. 2008 May;198(5):514.e1-8.
Boggess KA; Society for Maternal-Fetal Medicine Publications Committee. Maternal oral health in pregnancy. Obstet Gynecol. 2008 Apr;111(4):976-86.
Manau C, Echeverria A, Agueda A, Guerrero A, Echeverria JJ. Periodontal disease definition may determine the association between periodontitis and pregnancy outcomes. J Clin Periodontol. 2008 May;35(5):385-97.
|
||
|
A Brief History of Medicine
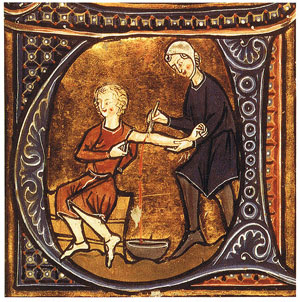
Physician letting blood from a patient. British Library, London. Photo courtesy of Wikimedia Commons |
|||
|
3000 BC. This mixture of roots and leaves will cure you.
2000 BC. Roots don't work well enough. If you're sick, sacrifice a goat.
0050 AD. Sacrifice is for pagans! If you want to get well, you must pray.
1000 AD. Prayer isn't enough. Some blood-letting will do you good.
1800 AD. Blood-letting weakens the patient. This potion will fix you up.
1900 AD. Potions are pure quackery. Here, swallow this pill.
1950 AD. Pills don't work. Now we have antibiotics.
2010 AD. Antibiotics can cause more harm than good. Here, take this mixture of roots and leaves.
Author unknown
|
|||
|
Do you have friends who would like this newsletter? If so, please feel free to share this newsletter with them.
If this newsletter was forwarded to you by a friend and you would like to subscribe, click here.
Copyright © 2010, Bruce Fife. All rights reserved.
|
|||